RESEARCH ARTICLE
Knowledge and Perception Related to Telepharmacy Utilization Among Pharmacist Professional Students in Central Java, Indonesia: A Cross-Sectional Study
Academic Editor: Pilli Govindaiah
Sciences of Pharmacy|Vol. 5, Issue 2, pp. 123-128 (2026)
Received
Nov 28, 2025Revised
Feb 19, 2026Accepted
Apr 13, 2026Published
Apr 21, 2026
Abstract
Introduction
Telepharmacy, as a component of telehealth, enables pharmacists to deliver pharmaceutical services remotely using information and communication technologies. The rapid advancement of digital health, particularly following the COVID-19 pandemic, has accelerated the global adoption of telepharmacy. However, its implementation remains limited and uneven, especially in developing countries such as Indonesia. Previous studies have identified knowledge and perception as key factors influencing the adoption of digital health technologies. However, findings in Indonesia remain inconsistent. Some studies report low levels of knowledge among pharmacy students, while others indicate increasing awareness. Despite these developments, evidence examining whether knowledge and perception are associated with actual telepharmacy utilization remains limited. Therefore, this study aims to examine the association between knowledge, perception, and telepharmacy utilization among pharmacy students in Central Java. It is hypothesized that knowledge is associated with telepharmacy utilization, while perception may not be directly associated with actual use (1, 2).
The development of information and communication technology has brought significant changes to various fields, including healthcare. One important innovation in healthcare is telepharmacy, which is defined as technology-based remote pharmaceutical services provided by registered pharmacists to patients (3). Telepharmacy allows pharmacists to provide information and supervision regarding medication use without meeting patients directly, thereby improving the accessibility and efficiency of healthcare services (4). The adoption of telepharmacy in the Asia-Pacific region is showing rapid growth, with Indonesia experiencing a more than doubling in usage to 51% in 2021 (3). Telepharmacy allows pharmacists to provide information and supervision regarding medication use without meeting patients directly, thereby improving the accessibility and efficiency of healthcare services (4). Telepharmacy adoption in the Asia-Pacific region is showing rapid growth, with Indonesia experiencing a more than doubling in usage to 51% in 2021 (5).
Despite its considerable potential, the implementation of telepharmacy in Indonesia continues to face several challenges, including limited knowledge and suboptimal perception among the public and prospective healthcare professionals (6). Previous studies among pharmacy students in major Indonesian cities reported that only 13.2% demonstrated adequate knowledge of telepharmacy (6). Similar findings have been observed in other settings, such as Ethiopia, where only 32.4% of pharmacy students had sufficient knowledge (7). This limited level of knowledge may represent a significant barrier to the effective adoption and implementation of telepharmacy services.
The mismatch between high positive perception and insufficient knowledge raises concerns that telepharmacy adoption may lack a strong competency foundation. This underscores the need for focused research among pharmacy students to examine whether perception alone is insufficient to support appropriate and responsible telepharmacy use (8).
Methodology
This study employed a cross-sectional design with purposive non-probability sampling. Data were collected from March to May 2024 among pharmacy professional students in Central Java, Indonesia. Ethical clearance was obtained from the Health Research Ethics Commission of the Faculty of Medicine, Sultan Agung Islamic University (No. 123/EC/KEPK/FK/UNISSULA/2024). Inclusion criteria included students enrolled in pharmacy professional programs who had internet access and provided informed consent. Incomplete responses were excluded from the analysis (9, 10).
The questionnaire was adapted from previously validated instruments and underwent forward–backward translation. Reliability testing demonstrated acceptable internal consistency (Cronbach’s alpha > 0.70). Knowledge scores were categorized into three levels based on total score distribution: low (10–20), moderate (21–30), and high (31–40). Perception was assessed using Likert-scale items and categorized as negative (13–32) or positive (33–52).
Telepharmacy utilization was defined as prior exposure to or engagement in telepharmacy-related activities. Bivariate analysis was performed using the Chi-square test to assess associations between knowledge, perception, and telepharmacy utilization. A p-value of < 0.05 was considered statistically significant. Effect size was evaluated using Cramer’s V (11).
Results and Discussion
Respondent Characteristics
A total of 219 pharmacy professional students participated in this study. The majority of respondents are female (77.6%) and aged 22-24 years (88.1%), as shown in Figure 1. Respondents were distributed almost evenly across the four universities surveyed. Female respondents dominated the completion of the research questionnaire. This is consistent with research conducted, which shows that graduates of pharmacy bachelor's degrees and the pharmacy profession are predominantly female. This is because the Pharmacy major is more popular with women than men. This result is also in line with the research (12–14), which shows that national data indicates women are expected to represent approximately 86% of pharmacists in Indonesia by 2030, and global analysis shows that from 2006 to 2023, the representation of women in the pharmaceutical workforce has increased significantly, with projections that by 2030 more than 70% of the world's pharmacists will be female (15). Respondents aged 20-25 years had the highest percentage in that study. That age is adulthood or young adulthood, where individuals have responsibility for their actions, attitudes, and desires and are not dependent on others (16).
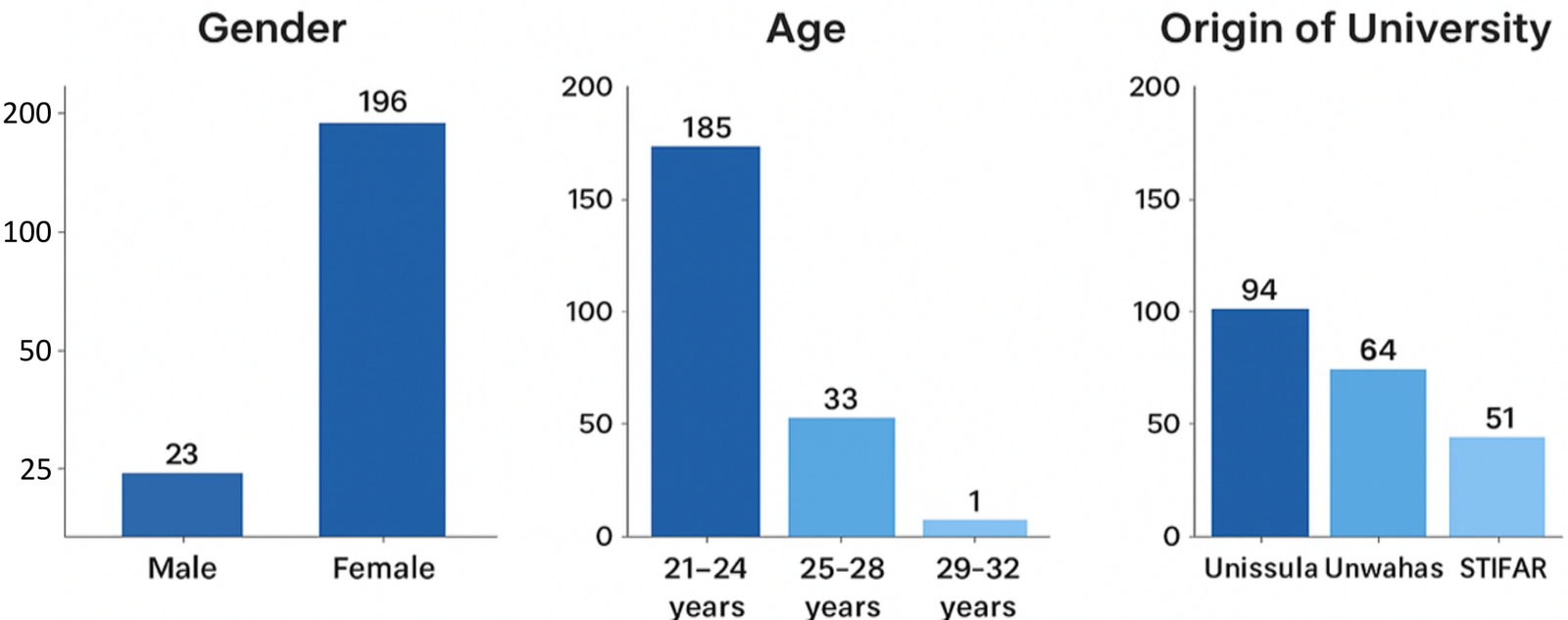
Distribution of Knowledge and Perception
A total of 219 respondents participated in this study. The majority were female (77.6%) and aged 22–24 years (88.1%). Most respondents had high knowledge (75.8%) and positive perception (96.8%). However, only 36.1% reported telepharmacy use. A statistically significant association was found between knowledge and telepharmacy use (χ² = 5.62, df = 2, p = 0.018), with a small effect size (Cramer’s V = 0.16). No significant association was found between perception and telepharmacy use (p = 0.451). This research for the respondent's knowledge category is divided into high, medium, and low, where high knowledge is said to have a score range of 76-100, medium 51-75, and low if < 51. In addition, for perception, it is said to be high if in the range of 68-100, medium in the range of 34-67, and low if in the range ≤33.
| Variable | Category | Score range | Frequency (n)% |
|---|---|---|---|
| Knowledge | Low | 10-20 | 12 (5.4) |
| Moderate | 21-30 | 41 (18.7) | |
| High | 31-40 | 166 (75.8) | |
| Perception | Negative | 13-32 | 7 (3.2) |
| Positive | 33-52 | 212 (96.8) | |
| Never | - | 140 (63.9) | |
| Use | - | 79 (36) | |
| Total | 219 (100) | ||
Based on the Table 1, it shows that 219 respondents have a high level of knowledge, with 166 (75.8%) respondents, and a moderate level of knowledge, with 53 (24.2%) respondents. Respondents with a positive perception are 212 (96.8%), and those with a negative perception are 7 (3.2%). The higher the level of knowledge of pharmacy students about telepharmacy, the greater the likelihood that pharmacy students will use telepharmacy services in pharmaceutical practice. This result is consistent with previous research showing that good knowledge can promote the implementation of telepharmacy in pharmacy practice (17).
The research results show that although most pharmacy students have a high level of knowledge and perception of telepharmacy, the actual usage rate of telepharmacy remains low. This indicates a gap between cognitive readiness and actual practice. Some of the hindering factors are the lack of access to hands-on practice (18). Another inhibiting factor is trust in data security, where the level of student trust in the security of patient information and privacy on the telepharmacy platform can affect their interest in using it. (19), Additionally, internet connectivity issues in remote areas also pose a challenge to the use of telepharmacy (20).
| Variable | Use of Telepharmacy | Total | |
|---|---|---|---|
| Use (n) | Never (n) | ||
| Knowledge | |||
| Low | 2 | 10 | 219 |
| Moderate | 12 | 29 | |
| High | 65 | 101 | |
| Perception | |||
| Negative | 2 | 5 | 219 |
| Positive | 77 | 135 | |
| Chi-square (χ²) = 5.62; df = 2; p = 0.018; Cramer’s V = 0.16 (Small effect) | |||
This study found that knowledge was significantly associated with telepharmacy utilization, although the strength of the association was small. Due to the cross-sectional design, causality cannot be inferred. The high proportion of positive perception (96.8%) may indicate a ceiling effect and potential social desirability bias.
This aligns with constructivist theory, where knowledge actively constructed through education and experience forms the basis for a person's actions (21). Students who understand the concepts, benefits, and workings of telepharmacy are more likely to be confident in trying it. The results of this study are consistent with the research (22). Based on the statistical test, the p-value obtained was 0.001, indicating a relationship between knowledge and the implementation of telepharmacy by pharmacists in pharmaceutical services. This indirectly suggests a relationship between the level of knowledge regarding the use of telepharmacy in pharmaceutical services within the community (23). This is in line with the research (24). revealed that in the knowledge level analysis, the majority of pharmacy students and pharmacy professionals had good knowledge about "Telepharmacy improves access to pharmacy services in areas with a limited number of pharmacists," with an average score of 98.64%. Interestingly, despite the very high positive perception (96.8%), this did not significantly correlate with actual usage (p=0.451). This shows that positive perception alone is not enough to change behavior. This finding aligns with Bruner's theory of perception, which states that perception is influenced by knowledge but also by other external factors (25).
These results are also in line with research (26), which was conducted on pharmacy students in Saudi Arabia who had a positive perception of 90%. The gap between attitude (positive perception) and behavior (use) may be caused by various external barriers that were not measured in this study, such as limited access to technology, cost, lack of practical opportunities, or the absence of clear regulations regarding telepharmacy (27). Students might find telepharmacy good and beneficial, but they don't use it because there's no immediate need or they don't know how to access it. This phenomenon can be explained by the presence of other more dominant factors influencing usage, such as attitudes, personal experiences, and preferences for conventional services (28). The results of this study are consistent with the research (29) which found that perception does not directly drive the use of digital healthcare services.
The practical implication of this research is the importance of improving the more applied educational aspects of the curriculum. Pharmacy education should not only focus on forming positive perceptions but should also provide direct experience or simulations of using telepharmacy so that students are prepared to adopt it in professional practice (30).
Other factors not covered in this study that could influence pharmacy students’ use of telepharmacy have also been highlighted in several international studies. Personal experience with digital or health-related technology has been shown to play a significant role in user acceptance. A study conducted in the United States found that prior familiarity with telepharmacy platforms significantly increased students’ willingness to adopt telepharmacy services because they felt more confident in navigating digital tools (31). Trust in data security and privacy protection is another important factor. Research in Saudi Arabia reported that pharmacy students’ intention to use telepharmacy was strongly influenced by their perceived security of patient information; concerns about data breaches reduced their readiness to use digital health platforms (32).
Furthermore, a number of foreign researchers have found that professional attitudes and ethical duty are significant variables. Because they are aware of their responsibilities for patient safety and confidentiality, pharmacy students who have a solid grasp of professional ethics are typically more careful when using new technology, such as telepharmacy. Another important factor is peer influence. According to a Malaysian study, peer recommendations and cooperative learning settings using health technology greatly boosted students' use of telepharmacy (33). These results suggest that students' adoption of telepharmacy might be influenced by social, ethical, and experiential aspects in addition to knowledge and perception.
It's also critical to take this study's shortcomings into account. The results may not be as broadly applicable as they could be because the study was limited to four pharmacy programs in Central Java province. International research also highlights how institutional infrastructure, curriculum design, and exposure to digital health systems contribute to regional variations in telepharmacy uptake. Therefore, to have a more thorough knowledge of pharmacy students' adoption of telepharmacy in Indonesia, more research with a larger sample across several provinces or national-level representation is required.
Conclusion
Knowledge was significantly associated with telepharmacy utilization among pharmacy students, whereas perception was not significantly related. However, the strength of the association was weak, indicating limited practical significance. These findings should be interpreted in light of several limitations, including the use of non-probability sampling, self-reported data, and the absence of multivariate analysis to control for potential confounders. Future studies employing more robust study designs and incorporating additional variables are recommended to provide a more comprehensive understanding of telepharmacy adoption.
Declarations
Conflict of Interest
The authors declare no conflicting interest.
Data Availability
All data generated or analyzed during this study are included in this published article.
Ethics Statement
This observational study was approved by the [No. 123/EC/KEPK/FK/UNISSULA/2024]. Written informed consent was obtained from all participants.
Funding Information
The work was funded by LPPM UNISSULA with grant number 54/8.USA-LPPM/VIIU2O25.
References
- Alexander E, Butler CD, Darr A, Jenkins MT, Long RD, Shipman CJ, et al. ASHP Statement on Telepharmacy. American Journal of Health-System Pharmacy. 2017;74(9):e236-e241. doi: https://doi.org/10.2146/ajhp170039
- Ahmed NJ, Almalki ZS, Alsawadi AH, Alturki AA, Bakarman AH, Almuaddi AM, et al. Knowledge, perceptions, and readiness of telepharmacy among community pharmacists. Saudi Pharmaceutical Journal. 2023;31(9):101713. doi: https://doi.org/10.1016/j.jsps.2023.101713
- Rahayu FR, Ramadhan IS, Hendriani R. Review Artikel : Pelaksanaan Telefarmasi Pada Pelayanan Kefarmasian Di Farmasi Komunitas. Jps. 2023;6(1):273-280. doi: https://doi.org/10.36490/journal-jps.com.v6i1.60
- Poudel A, Nissen L. Telepharmacy: a pharmacist’s perspective on the clinical benefits and challenges. Iprp. 2016;Volume 5:75-82. doi: https://doi.org/10.2147/iprp.s101685
- Almeman A. The digital transformation in pharmacy: embracing online platforms and the cosmeceutical paradigm shift. J Health Popul Nutr. 2024;43(1). doi: https://doi.org/10.1186/s41043-024-00550-2
- Alfian SD, Khoiry QA, Andhika A. Pratama M, Pradipta IS, Kristina SA, Zairina E, et al. Knowledge, perception, and willingness to provide telepharmacy services among pharmacy students: a multicenter cross-sectional study in Indonesia. BMC Med Educ. 2023;23(1). doi: https://doi.org/10.1186/s12909-023-04790-4
- Tegegne MD, Wubante SM, Melaku MS, Mengiste ND, Fentahun A, Zemene W, et al. Tele-pharmacy perception, knowledge and associated factors among pharmacy students in northwest Ethiopia: an input for implementers. BMC Med Educ. 2023;23(1). doi: https://doi.org/10.1186/s12909-023-04111-9
- Ahmed NJ, Almalki ZS, Alsawadi AH, Alturki AA, Bakarman AH, Almuaddi AM, et al. Knowledge, Perceptions, and Readiness of Telepharmacy among Hospital Pharmacists in Saudi Arabia. Healthcare. 2023;11(8):1087. doi: https://doi.org/10.3390/healthcare11081087
- Wang X, Cheng Z. Cross-Sectional Studies. Chest. 2020;158(1):S65-S71. doi: https://doi.org/10.1016/j.chest.2020.03.012
- Pérez-Guerrero EE, Guillén-Medina MR, Márquez-Sandoval F, Vera-Cruz JM, Gallegos-Arreola MP, Rico-Méndez MA, et al. Methodological and Statistical Considerations for Cross-Sectional, Case–Control, and Cohort Studies. Jcm. 2024;13(14):4005. doi: https://doi.org/10.3390/jcm13144005
- Sadiq M, Mehmood T, Aslam M. Identifying the factors associated with cesarean section modeled with categorical correlation coefficients in partial least squares. PLoS ONE. 2019;14(7):e0219427. doi: https://doi.org/10.1371/journal.pone.0219427
- Popovici I, Carvajal MJ. Is Pharmacy a Friendly Profession for Everyone in the U.S.? A Probe into Gender and Other Income Disparities. Pharmacy. 2025;13(2):49. doi: https://doi.org/10.3390/pharmacy13020049
- Meilianti S, Smith F, Kristianto F, Himawan R, Ernawati DK, Naya R, et al. A national analysis of the pharmacy workforce in Indonesia. Hum Resour Health. 2022;20(1). doi: https://doi.org/10.1186/s12960-022-00767-4
- Janzen D, Fitzpatrick K, Jensen K, Suveges L. Women in pharmacy. Can Pharm J. 2013;146(2):109-116. doi: https://doi.org/10.1177/1715163513481323
- Hayatul Millah. Strategi pemasaran dalam menghadapi persaingan usaha prespektif etika bisnis islam. AlIdarah.j.man.bus.is. 2020;1(2):13-21. doi: https://doi.org/10.35316/idarah.2020.v1i2.13-21
- Tjiptoatmadja NN, Alfian SD. Knowledge, Perception, and Willingness to Use Telepharmacy Among the General Population in Indonesia. Front. Public Health. 2022;10. doi: https://doi.org/10.3389/fpubh.2022.825554
- Rasdianah N, Djuwarno EN, Lasimpala NI, Suryadi AMA, Madania M. Persespi Tenaga Farmasi Tentang Telefarmasi di Apotek Kota Gorontalo. Jccp. 2024;1(2):13-18. doi: https://doi.org/10.70075/jccp.v1i2.28
- Naima FU, Sukorini AI, Hermansyah A. Identifikasi Faktor Pendukung dan Penghambat Aktivitas Apoteker di Media Sosial dalam Menunjang Praktik Kefarmasian. Jfiki. 2021;7(1SI):55. doi: https://doi.org/10.20473/jfiki.v7i1si2020.55-62
- Lelyana N. Dampak telemedis terhadap akses pelayanan kesehatan di masyarakat pedesaan. Jurnal Ilmiah Kedokteran. 2024;3(2):78-89. doi: https://doi.org/10.55080/mjn.v3i2.832
- I Dewa Ayu Eka Purba Dharma Tari. Flourishing mahasiswa: perspektif teori konstruktivisme jean peaget. Js. 2024;8(2):1951-1961. doi: https://doi.org/10.36526/santhet.v8i2.4533
- Wiryani LSU, Iswandi I, Herdwiani W. The Relationship of the Level of Pharmacy's Knowledge in Telepharmacy on Pharmaceutical Services in Pharmacy in Denpasar City Bali Indonesia. Ijmmu. 2023;10(10):458. doi: https://doi.org/10.18415/ijmmu.v10i10.5196
- Retnowati E, Primananda AZ, Manik N, Isnaini RD, Harahap F. Tingkat pengetahuan penggunaan telefarmasi dalam pelayanan kefarmasian di masyarakat. ijf indonesia j. farm. 2025;9(2):73-80. doi: https://doi.org/10.26751/ijf.v9i2.2626
- Ilma DL, Mustikaningtias I, Salsabila IYN, Sholihat NK, Parmasari DH. Analisis Tingkat Pengetahuan, Sikap dan Perilaku Apoteker Terkait Penggunaan Telefarmasi: Studi Cross-Sectional. J. Pharm. Sci. Clin. Res. 2023;8(2):179. doi: https://doi.org/10.20961/jpscr.v8i2.65680
- Banowati AD, Kristina SA, Puspandari DA. Hubungan Persepsi Telemedicine dengan Kesediaan Menggunakan Telemedicine Pada Mahasiswa Farmasi Yogyakarta. Majalah Farmaseutik. 2024;19(4):591. doi: https://doi.org/10.22146/farmaseutik.v19i4.85001
- Albarrak AI, Mohammed R, Almarshoud N, Almujalli L, Aljaeed R, Altuwaijiri S, et al. Assessment of physician’s knowledge, perception and willingness of telemedicine in Riyadh region, Saudi Arabia. Journal of Infection and Public Health. 2021;14(1):97-102. doi: https://doi.org/10.1016/j.jiph.2019.04.006
- Sasanti AD, Maharani L, Sholihat NK, Purwonugroho TA, Mustikaningtias I, Ilma DL. Analisis Kualitatif Mengenai Peran dan Perilaku Apoteker di Apotek Terkait Penggunaan Telefarmasi Selama Pandemi COVID-19. J. Pharm. Sci. Clin. Res. 2022;7(2):149. doi: https://doi.org/10.20961/jpscr.v7i2.55878
- Damayanti F, Ascobat Gani. Hubungan Pemanfaatan Telemedicine Dengan Peningkatan Kepuasan Pasien, Kepatuhan Pasien Berobat dan Loyalitas Pasien di Rumah Sakit. Sljil. 2024;6(3):1085-1100. doi: https://doi.org/10.46799/syntax-idea.v6i3.3038
- Novita W. Perilaku penggunaan platform kesehatan digital selama pandemi COVID-19. J Manaj Akunt. 2023;17(3):288–297.
- Naufal M, Yuwindry I, Rizali M. Persepsi Apoteker Tentang Penerapan Telefarmasi Di Apotek. pharmaceutical care and science. 2023;3(2):109-114. doi: https://doi.org/10.33859/jpcs.v3i2.249
- Alowais M, Rudd G, Besa V, Nazar H, Shah T, Tolley C. Digital literacy in undergraduate pharmacy education: a scoping review. Journal of the American Medical Informatics Association. 2023;31(3):732-745. doi: https://doi.org/10.1093/jamia/ocad223
- Mekurianew Kelkay J, Wubneh HD, Beri HM, Tefera AM, Molla RA, Negatu AA. Adoption of telepharmacy among pharmacists, physicians, and nurses at Hawassa City Public Hospitals, Ethiopia. PLOS Digit Health. 2024;3(12):e0000693. doi: https://doi.org/10.1371/journal.pdig.0000693