RESEARCH ARTICLE
Comparison of Blood Glucose Control Among Type 2 Diabetics Consuming Oral Antidiabetic Drug Versus Oral Antidiabetic Drug With Home Remedies
Sciences of Phytochemistry|Vol. 2, Issue 1, pp. 1-6 (2023)
Received
Dec 21, 2022Revised
Dec 29, 2022Accepted
Dec 30, 2022Published
Jan 12, 2023
Abstract
Introduction
Changing lifestyles have led to reduced physical activity and increased obesity which has made diabetes mellitus to become one of the most chronic-long term diseases in the world, which is increasing in number as years are passing (1). The prevalence of diabetes, deaths attributable to diabetes, and health expenditure associated with the treatment of diabetes continue to raise across the globe with important social, financial, and health system implications (2). Many plants with medicinal properties have been explored for their useful effect in different types of diabetes, as an alternative to antidiabetic oral drugs. Plants are providing prospective results in controlling the blood glucose level and are widely used in several traditional systems of medicine to prevent and control diabetes (3).
Type 2 Diabetes is a serious, chronic disease that occurs either when the body cannot use insulin which is produced by the pancreas, or when the pancreas itself does not produce enough amount of insulin (a hormone that regulates blood glucose). Hyperglycemia, as a result of uncontrolled diabetes mellitus, may lead to serious heart, kidney, or other vital organ diseases. More than 420 million people around the world are suffering from diabetes mellitus (4). Globally, an estimated 422 million adults were living with diabetes in 2014, compared to 108 million in 1980. A rise in the prevalence (age-standardized) of diabetes has doubled since 1980, rising from 4.7% to 8.5% in the adult population globally. This shows an elevation in risk factors associated with it such as being overweight and obese. Over the past decade, the prevalence of diabetes has risen faster in low- and middle-income countries as compared to high-income countries (4). No longer a disease of predominantly rich nations, the prevalence of diabetes is steadily increasing everywhere, most markedly in the world’s middle-income countries. When diabetes is uncontrolled, it has dire consequences for health and well-being. The total prevalence in 2017 in India was 8.8% and it is estimated to reach 11.4%. Type 2 diabetes is mostly seen in older adults, but it is increasingly seen in children, adolescents, and younger adults due to rising levels of obesity, physical inactivity, and poor diet (5). Prevalence and risk factors of diabetes in the adult population of South Asia ranged from 0.9% in Bangladesh to 21.2% in India. The highest prevalence was observed in urban areas showing rapid urbanization, which plays a major role in the increased prevalence. However, the results also indicate that the prevalence of diabetes is on the rise even in rural areas. Although not a single determinant is responsible for the high prevalence, a complex interaction of different factors plays a part in the increased prevalence of diabetes in South Asia. (6)
Persistently high blood glucose levels cause generalized vascular damage affecting the heart, eyes, kidneys, and nerves. Diabetes is one of the leading causes of cardiovascular disease (CVD), blindness, kidney failure, and lower-limb amputation (5). An estimated 1.6 million deaths were directly caused because of diabetes alone in 2015. It caused a further 2.2 million deaths due to a rise in blood sugar levels in 2012. Almost fifty percent of all deaths were caused due to diabetes occurring before the age of 70 years. Diabetes will be the seventh leading cause of death in 2030 as per WHO projection. Maintaining a body weight within the normal range of body mass index, a healthy and nutritious diet, regular physical activity, and avoiding tobacco and alcohol consumption are ways to prevent or delay the onset of type 2 diabetes. Diabetes can be controlled, and its aftermath is delayed or avoided with a balanced diet, regular physical activity, medication, regular screening, and treatment for complications (7).
Many herbs have been shown to have antidiabetic activity by regulating insulin secretion, insulin sensitivity to the cells, glucose abruption, etc. to improve the glycemic control of the patients. In addition to glycemic control, some herbs depicted effectiveness in controlling cardiovascular complications by reducing TG, cholesterol levels, and BMI (8). Alternative to synthetic agents, plants provided a potential source of hypoglycemic drugs and are widely used in several traditional systems of medicine to prevent and manage diabetes. Other alternative therapies such as dietary supplements, yoga therapy, hydrotherapy, and acupuncture are less likely to have the side effects of conventional approaches for diabetes (3).
This research intends to compare blood glucose control in type 2 diabetics on oral antidiabetic drugs versus oral antidiabetic drugs with home remedies and to understand whether home remedies are giving any added benefits in glucose control instead of consuming oral antidiabetic drugs alone for the treatment of type 2 diabetes. This research will advance our understanding on the trends in diabetes prevalence and the actions that can be taken to prevent and control diabetes. Through this study, we hope to give better awareness of the disease and improvement in dietary choices and lifestyle practices thereby helping diabetic patients to manage diabetes.
Materials and Methods
A cross-sectional study was undertaken on 300 patients attending OPD. Purposive sampling (non-probability) was done keeping in mind the exclusion and inclusion criteria with people having type 2 diabetes who visited OPD of Medicine, Kasturba Medical College & Hospital, Manipal. Inclusion criteria for recruitment were type 2 diabetics between the age groups 30-70, and type 2 diabetics diagnosed for more than 1 year. Exclusion criteria were type 2 diabetics on Insulin, recently diagnosed type 2 diabetics, and type 2 diabetics with any other co-morbidities. The research topic was selected based on a literature review. Preparation and submission of the final project protocol to the Institutional ethical committee were completed as per guidelines. After IEC and CTRI approval (Approval number CTRI/2018/06/014590), participants were recruited as per inclusion criteria and were given the participation information sheet and a brief explanation of the study was done. During the first visit, the consent form was taken, and data was collected with a semi-structured validated questionnaire which included diet, home remedies, family history, lifestyle, socio-demography, medical history, and anthropometric measurements. After the consent of patients and assessment of the questionnaire, patients were divided into only oral antidiabetic drug and oral antidiabetic drug with home remedies group. Around 60 minutes were spent with each patient when they came for their regular checkups and the data collection. Biochemical parameters like FBS, PPBS, RBS, and HbA1c were analyzed from the subject’s hospital records and a dietary assessment was done using a 24-hour food recall. Their dietary pattern was assessed with a food frequency questionnaire. The quantifications of food were done through measurement of cups and spoons and they were recorded accordingly. An education material that explained the management of diabetes was provided to all the participants. All the subjects were given effective counselling and were asked to follow the guidelines. The collected data were processed with the DietCal (version 8.0) software and the SPSS (version 16.0) software. The processed data were analyzed by correlation, regression, Chi-square, and T-test. The results obtained were carefully interpreted and conclusions were drawn based on the findings.
Results
This was an observational study. A total of 300 samples were interviewed during the period of data collection from June 2018- October 2018 with a semi-structured validated questionnaire. Figure 1 shows the distribution of the study of 300 patients into 2 groups. Diabetics with home remedies usage (also called as HM) are 127 (42.3%) and without home remedies usage (also called as WHM) are 173 (.57.7 %). Figure 2 shows the types of home remedies used and the percentage of usage of each home remedy in the study population.
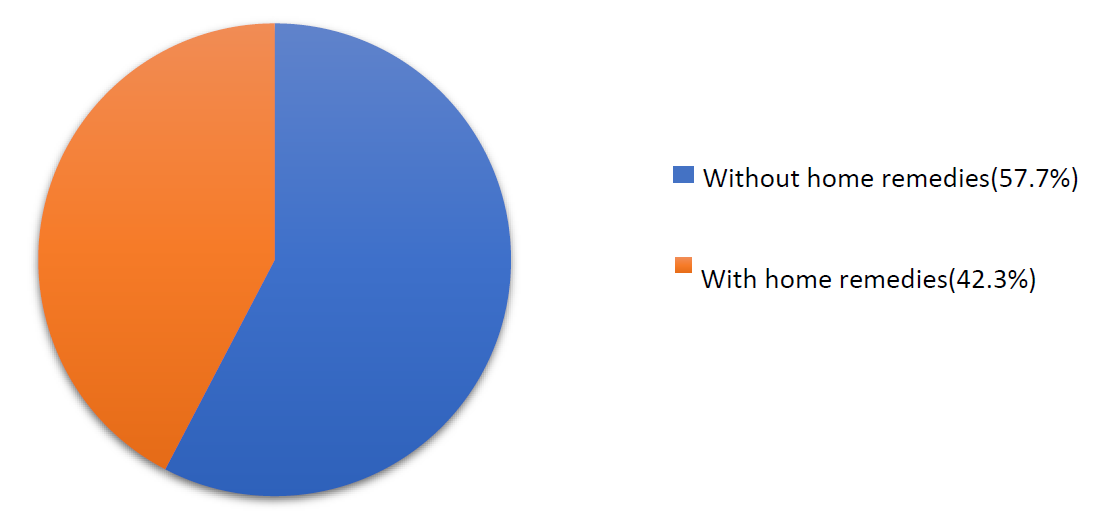
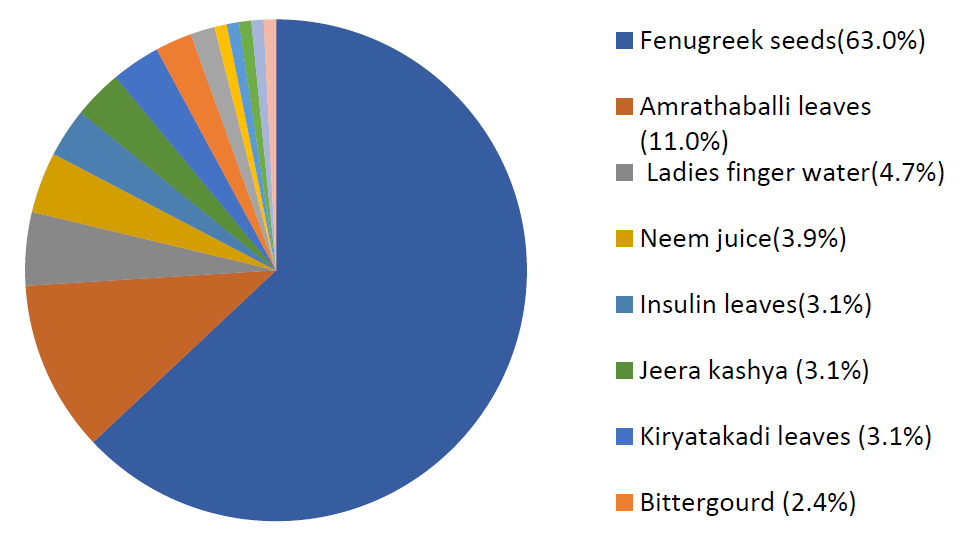
Anthropometric assessments such as height, weight, waist circumference, and hip measurements were measured using standard procedures. Body mass index and waist-hip ratio were then calculated. The mean BMI was found to be (25.3 ± 4.1717). Out of 300 patients, most of the patients 106 (35.3%) are in the obese I category, followed by 81 (27%) in the normal weight category, 62 (20.7%) in the overweight category, 45 (15%) in obese II, and 6 (2%) in the underweight category. In the waist: hip ratio category, a majority of 242 (80.7%) of all patients fall under the risk category followed by normal 58 (19.3%).
The physical activity of all the patients was recorded by recording their daily activity for a normal day and then the PAL value was calculated with the factorial method and classified as per ICMR. The physical activity classification shows a majority of 143 (47.7%) fall under very light activity, 135 (45%) fall under sedentary, 20 (6.7%) fall under Active and 2 (0.7%) fall under the vigorous category.
A comparative analysis of the blood glucose level of type 2 Diabetics who are on oral antidiabetic drug v/s and those taking some home remedies along with oral antidiabetic drug was done by independent sample T-test. Table 1 shows the difference in blood glucose parameters between type 2 diabetics with and without home remedies.
There is no significant difference between the participants' dietary habits between the two groups. Table 2 showed that the mean energy, carbohydrate, protein, fat, total dietary fiber, and soluble and insoluble dietary fiber intake was almost similar in participants with home remedies as compared to the mean energy intake without home remedies, but the difference is not statistically significant.
| Parameters | Mean ± SD | t-value | p-value | 95% confidence interval | |
|---|---|---|---|---|---|
| FBS | With HR | 149.80 ± 56.576 | 0.889 | 0.577NS | (-7.375, 19.519) |
| Without HR | 155.87 ± 59.831 | ||||
| PPBS | With HR | 214.99 ± 82.811 | 1.671 | 0.179 NS | (-3.103, 38.043) |
| Without HR | 232.46 ± 94.040 | ||||
| HbA1C | With HR | 7.909 ± 1.9488 | 0.919 | 0.413 NS | (-0.2452, 0.6748) |
| Without HR | 8.123 ± 2.0370 | ||||
| Nutrients | Mean ± SD | t-value | p-value | 95% CI | |
|---|---|---|---|---|---|
| Energy Adequacy | With HR | 125.9582 ± 20.87520 | 0.664 | 0.507 NS | -3.34384, 6.54584 |
| Without HR | 127.6092± 21.58139 | ||||
| Carbohydrate Adequacy | With HR | 119.9033± 17.91971 | 0.796 | 0.427 NS | -2.57760, 6.08081 |
| Without HR | 121.6549± 19.46306 | ||||
| ProteinAdequacy | With HR | 144.2047± 41.52936 | -0.019 | 0.985 NS | -9.38250, 9.20427 |
| Without HR | 144.1156± 39.57549 | ||||
| FatAdequacy | With HR | 125.0394± 34.05817 | 0.523 | 0.601 NS | -5.83062, 10.0526 |
| Without HR | 127.1503± 34.87937 | ||||
| Dietary fiberAdequacy | With HR | 149.5433± 47.45988 | 0.185 | 0.854 NS | -9.03703, 11.17836 |
| Without HR | 150.4798± 40.11141 | ||||
| Insoluble DFAdequacy | With HR | 234.0079± 79.76787 | 0.133 | 0.895 NS | -15.72997,-18.00324 |
| Without HR | 235.1445± 68.25931 | ||||
| Soluble DFAdequacy | With HR | 65.0472 ± 17.04702 | 0.333 | 0.739NS | -2.91736, 4.10611 |
| Without HR | 65.6416 ± 13.82612 | ||||
The glycemic load of the food was calculated from the 24-hour diet recall of the participant. The independent sample T-test showed no significant difference in the mean glycemic load of the diet between participants of the 2 groups (t value 0.450, p-value 0.653NS). The mean value is almost similar for without and with HR, as shown in Table 3. Both groups consumed diets with very high glycemic loads.
| Parameters | Mean ± SD | T-value | p-value | 95% confidence interval | |
|---|---|---|---|---|---|
| Glycemic load | With HR | 254.17 ± 62.03365 | -0.450 | 0.653 NS | (-16.13416, 10.13314) |
| Without HR | 257.17 ± 53.22020 | ||||
Details of socio-demographic factors- age, religion, place of residence, education, occupation, family income, and SES class were recorded and analyzed. The Chi-square test showed no significant association in mean socio-demographic factors on blood glucose levels such as FBS, PPBS, and HbA1c in participants with home remedies and without home remedies at a 5% level of significance (p ≥ 0.05)
Lifestyle habits like smoking, consumption of alcohol, and consumption of tobacco showed no impact on the blood glucose level. The Chi-square test showed no significant association between smoking habit, consumption of alcohol, consumption of tobacco, and blood glucose level (FBS, PPBS, HbA1c) in participants with home remedies and without home remedies at a 5% level of significance (p ≥ 0.05).
Waist and hip circumference and height and weight were recorded, and the BMI and waist-to-hip ratio were calculated and analyzed. The correlation test showed no significant association between mean BMI, weight, waist circumference and waist-hip ratio, PAL, and HbA1c in participants with home remedies and without home remedies at a 5% significance level.
Discussion
Blood sugar levels can be controlled through lifestyle interventions that focus on increasing physical activity and adopting a healthy diet (9). Importance must be given to promoting a healthier lifestyle, weight loss, adopting a healthy dietary pattern, and finding solutions that will elevate the increase in compliance and adherence to lifestyle changes.
Diet has been recognized as a foundation in the management of diabetes mellitus. Intake of carbohydrates with a high glycemic index (a relative measure of the incremental glucose response per gram of carbohydrate) produces high insulin resistance than with a low glycemic index carbohydrate. Both glycemic load (the glycemic index multiplied by the amount of carbohydrates) and glycemic index of overall diet have been associated with a greater risk of type 2 Diabetes and increase insulin resistance in diabetics (9). Eating right plays an important role in the management of diabetes, especially for high-risk individuals (10). A combined approach that includes changes in pharmacological treatment, as well as lifestyle, is necessary. Choosing low glycemic index foods in place of conventional or high glycemic index foods has a small but clinically useful effect on medium-term glycemic control in patients with diabetes. An intake of carbohydrates with a high glycemic index produces greater insulin resistance than an intake of low-glycemic-index carbohydrates (11).
A simple dietary supplement such as fenugreek seed can help to control blood glucose but a balanced diet, exercise, and weight management are at the core of a management strategy and will improve the quality of life of diabetic patients. Short-term ingestion of fenugreek seeds 30 grams/day significantly decreased HbA1C levels in patients with uncontrolled diabetes (12).
Patients with type 2 diabetes that are choosing alternative therapies with anti-hyperglycemic effect are increasing and herbal medications are the most commonly used alternative therapy for glycemic control. Commonly used alternative therapies and herbal remedies are less likely to have side effects for type 2 diabetes than conventional approaches (13).
Some spices are known to show many beneficial physiological effects including the antidiabetic influence. Among the spices, fenugreek seeds (Trigonella foenumgraecum), turmeric (Curcuma longa), onion (Allium cepa), and garlic (Allium sativum) have been experimentally documented to possess antidiabetic potential. In a limited number of studies, cumin seeds (Cuminum cyminum), curry leaves (Murraya koenigii), coriander (Coriandrum sativum) mustard (Brassica nigra), and ginger (Zingiber officinale), have been reported to be hypoglycaemic (14).
Conclusion
There is no significant difference between mean blood glucose control in type 2 diabetics with oral antidiabetic drugs versus oral antidiabetic drugs with home remedies. However, the mean blood glucose levels in the participants with home remedies are lower compared to participants without home remedies. It is also seen that there is no difference between mean glycemic loads among the 2 groups which indicates poor control of diet in both groups. Diet and lifestyle modification are very important for glycemic control. Home remedies can give an added benefit if diet and lifestyle modification are followed which will prevent long-term complications. The study can be taken forward by doing a case-control study where the glycemic load of the diet is maintained to see if there is any change in blood glucose level with home remedies.
Abbreviations
HM – Home Remedies, WHM – Without Home Remedies, FBS – Fasting blood sugar, PPBS – Post Prandial Blood Sugar, RBS – Random Blood Sugar, HbA1C – Hemoglobin A1c, CVD – Cardio Vascular Disease, WHO – World Health Organization, BMI – Body Mass Index, OPD – Out Patient Department, PAL – Physical Activity Level.
Declarations
Conflict of Interest
The authors declare no conflicting interest.
Data Availability
The unpublished data is available upon request to the corresponding author.
Ethics Statement
The study and experimental design were approved by Institutional Ethical Committee of Manipul University and Clinical Trials Registry India with approval letter number of CTRI/2018/06/014590.
Funding Information
Not applicable.
References
- Shaw JE, Sicree RA, Zimmet PZ. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Research and Clinical Practice 2009;87(1):4-14.
- Ogurtsova K, Fernandes JD da Rocha, Huang Y, Linnenkamp U, Guariguata L, et al. IDF Diabetes Atlas: Global estimates for the prevalence of diabetes for 2015 and 2040. Diabetes Research and Clinical Practice 2017;128:40-50.
- Pandey A, Tripathi P, Pandey R, Srivastava R, Goswami S. Alternative therapies useful in the management of diabetes: A systematic review. Journal of Pharmacy & Bioallied Sciences 2011;3:504-512.
- World Health Organisation. Global Report on Diabetes. 2016; pp. 6-10. Available at: https://www.who.int/publications-detail-redirect/9789241565257.
- International Diabetes Federation. IDF Diabetes Atlas 8th ed, Nam Han Cho et al (eds) 2017; pp. 78-80.
- Kakar, Zaheer A, Siddiqui, Muhammad A, Amin, Rooh A. Prevalence and Risk Factors of Diabetes in Adult Population of South Asia. Clinical Medicine and Diagnostics 2013;3:18-28.
- World Health Organization. Diabetes. Available at: http://www.who.int/en/news-room/fact-sheets/detail/diabetes.
- Choudhary H, Pandey M, Hua C, Mun C, Jing, Jessmie K, et al. An update on natural compounds in the remedy of diabetes mellitus: A systematic review. Journal of Traditional and Complementary Medicine 2018;8:361-376.
- Walter W, Liu S, Manson J. Glycemic index, glycemic load, and risk of type 2 diabetes. The American Journal of Clinical Nutrition 2002;76:274-280.
- Asif M. The prevention and control the type-2 diabetes by changing lifestyle and dietary pattern. Journal of Education and Health Promotion 2014;3:2-5.
- Jennie B, Hayne S, Petocz P, Colagiuri S. Low–Glycemic Index Diets in the Management of Diabetes. Diabetes Care 2013;26:2261-2267.
- Hudson T. An Overview of the Research and Clinical Indications. 2010.
- Dey L, Attele A, Yuan C. Alternative Therapies for Type 2 Diabetes. Alternative Medicine Review 2001;7:45-58.
- Srinivasan K. Plant foods in the management of diabetes mellitus: Spices as beneficial antidiabetic food adjuncts. International Journal of Food Sciences and Nutrition 2005;56:399-414.
